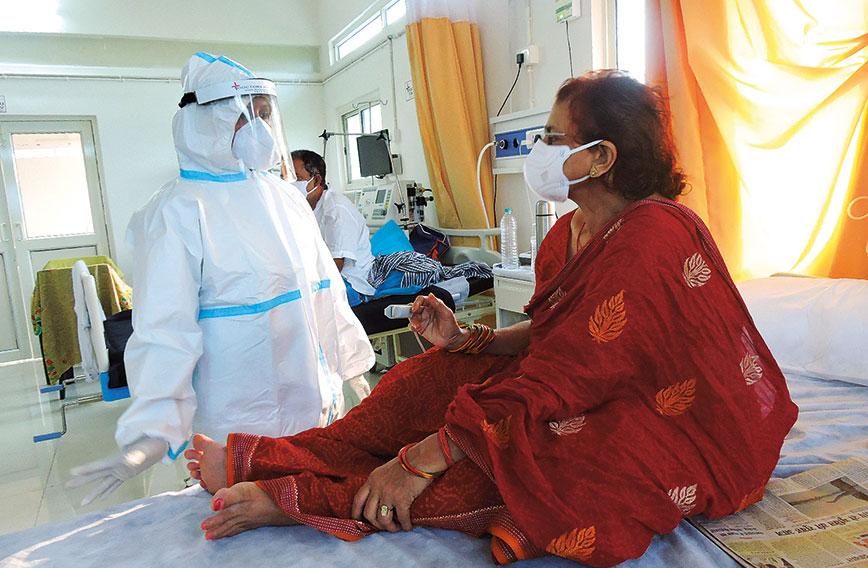
In the Masarhi hospital, facilities are as good as in a city hospital
The next pandemic?
By Dr Ravikant Singh
Masarhi is a village in Bihar so steeped in grinding poverty that its people are known to hunt rats in their fields and eat them. In the midst of the coronavirus pandemic, however, these hapless people with so little have what many residents in cities don’t — an easily accessible and affordable hospital with state-of-the-art facilities to treat patients sickened by the virus.
It is just a small 50-bed hospital and it began in 2015, much before the pandemic, as an even more modest community health centre set up by Doctors For You (DFY) after we helplessly watched an elderly resident of Masarhi die in his hut before he could be treated.
The small hospital now makes a world of difference to Masarhi, but back then all we at DFY wanted was to give the village and its nearby areas access to at least some basic care. The government-run primary health centre (PHC) that was meant to serve Masarhi was at a distance and in terrible shape. Patna, being the capital of Bihar, had hospitals and was merely 25 km away, but getting there meant a difficult journey of more than an hour because of broken roads and the absence of ready transportation.
WATCH THE VIDEO: https://www.youtube.com/embed/v0SuyCYzvBw
In the face of such odds, it was common for patients in Masarhi to die in their huts from diseases that could otherwise be easily diagnosed and treated. The death we witnessed prompted us to act.
As our health centre came up, it provided the villagers of Masarhi with options they had never had before. From pregnancies and deliveries and tracking child and maternal well-being to dealing with local outbreaks of diseases, the health centre brought important improvements to their neglected lives.
My colleague, Dr Taru Jindal, did most of the heavy lifting involved in setting up the health centre. She gave up her life in Mumbai and a teaching assignment to relocate to Masarhi. Engaging with the local people on a daily basis, she created new levels of awareness in them about their health.
Over time, what we planned as a simple health centre has acquired the dimensions of a miniature hospital. It is now called Vistex Hospital in recognition of the support we have got from Vistex Foundation, which has helped make possible Rs 3.8 crore in capital investments. It has annual running costs of Rs 84 lakh. There are six doctors and 12 nurses.
And with the pandemic suddenly coming upon us this small hospital has quite easily morphed into a facility for treating coronavirus patients. It has oxygen support, ICU capacities and treatment protocols that equal many urban facilities.
 Masarhi village: People live in abject poverty
Masarhi village: People live in abject poverty
In fact, the villagers of Masarhi are now, at least in this respect, better off than many of the residents of Patna, even though it has the exalted status of being the capital of Bihar and by contrast Masarhi is difficult to find on the map.
Healthcare infrastructure doesn’t get made overnight. It can, of course, come up quickly during a pandemic, as we have seen. But not with the same long-term benefits as a healthcare system designed to serve large numbers of people steadily and with equal access.
To build a dependable public health system calls for vision and commitment. It is like a giant jigsaw in which each piece has to be crafted to serve a combined purpose. Required are doctors, nurses, technicians, field staff, testing and diagnostic capabilities and hospitals, both big and small.
The Masarhi hospital is an example of what can be achieved with a sense of mission and purpose and professional involvement. It is donor-driven and patients are currently only charged a token fee of Rs 5. But over time, as it begins providing secondary care, we expect the hospital to become sustainable.
A public health system has to take shape through multiple such initiatives tied to a national objective of taking healthcare to the people who need it most. A big responsibility rests with the government, which must invest significantly more than the 1.3 percent of GDP that it currently does at the national level.
Hospitals like the one at Masarhi serve an important public purpose. But they come with inherent limitations, being dependent on donors and the spiritedness of physicians of the kind you will find associated with DFY. It is important that governments see the energy flowing here and use it creatively to grow a larger healthcare system. Finally, it is only the government that can provide the overarching structure for a broad-based healthcare system that a country with diverse patient loads like ours requires.
MOTIVATION NEEDED
At Masarhi we can handle 50 patients at a time. That is great, considering that there were no facilities available earlier. But it is not enough. DFY is currently managing coronavirus patients in 12 hospitals all over the country. Dr Rajat Jain, DFY president, has worked with other colleagues to set up facilities in Bengaluru and Delhi. Everywhere it is the same story of the healthcare system falling far short of requirements.
 Entry to the Masarhi hospital
Entry to the Masarhi hospital
The government would do well to rally around doctors, scientists, planners, funders, NGOs and community groups, and do so soon because there is no time to be lost. When governments are supportive and give a free hand to professionals, the results are immediately visible. An example is how Dr Suresh Kumar, in the midst of the pandemic, has transformed services at LNJP Hospital under the Aam Aadmi Party (AAP) government in Delhi.
Even as we struggle to cope with the current pandemic, it is clear that there could well be more pandemics on their way. Before the novel coronavirus, technically known as SARS-Cov-2, came along, there have been HIV, SARS-CoV, Nipah, Ebola, Zika, Swine Flu and going back further in time the devastating Spanish Flu.
A public health system has to have the strength and flexibility to measure up to such unpredictable outbreaks and also handle the disease burdens that exist in the normal course. In India think TB, cancer, dengue, malaria, heart disease, diabetes, HIV and more.
As a result of high consumption, exploitation of natural resources and global warming we now experience more natural disasters than ever before. Getting healthcare to everyone who needs it should be a national priority going much beyond the investments we see in private hospitals. The system as it exists is not just inadequate but teeters on the verge of collapse.
WUHAN TO PATNA
When my brother, who is a municipal employee in Patna, contracted COVID-19 recently, I took him to Masarhi for treatment, confident that he would be better-off there than in any Patna hospital. I treated him in Masarhi for two weeks and he was ready to go back to work though his was a severe case and not without some complications.
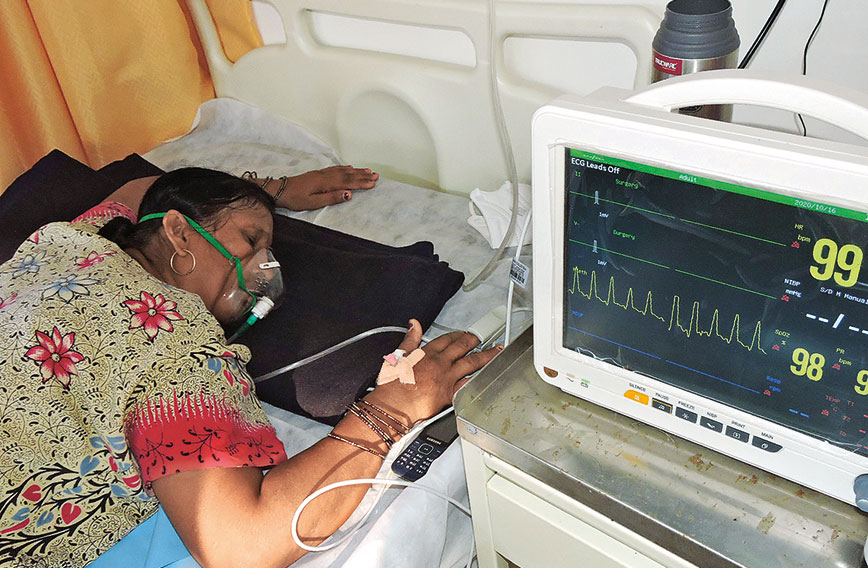 A patient is monitored and put in prone position in the Masarhi hospital
A patient is monitored and put in prone position in the Masarhi hospital
It is not the first time that I have had to take care of a family member in the middle of a much larger public health emergency. Last year, when Patna was flooded and my mother got infected with the dengue virus, I treated her in a makeshift clinic in a tent because hospitals were all under water.
In an interconnected world it doesn’t take long for a virus to show up at your doorstep, often having journeyed across the globe. It took no time at all for the novel coronavirus to get from Wuhan to Patna. The question no longer is whether we will have another epidemic or pandemic. It is when. We can’t afford to live in denial.
There are more than one million viruses on the planet with the potential of being transmitted from animals to human beings. If we see the pattern of emergence of highly infectious pathogens of pandemic potential over the past few decades, it is very clear that almost every decade has experienced two to three major outbreaks.
The World Health Organization (WHO) has recorded more than 5,000 major and minor disease alerts and one new disease outbreak each year.
The rat and bat are two major carriers of multiple deadly pathogens. The bat, being the second most common mammalian species, is a very good vector for thousands of viruses.
It is very difficult to exactly predict the date and location of an outbreak although we know the major hotspots where there is potential for an outbreak. But what we do know is that there is no substitute for perpetual preparedness.
CRISIS SPECIALISTS
I founded Doctors For You in 2007 at KEM Hospital when I was a post-graduate student to get people to donate blood platelets during a dengue outbreak in Mumbai. But the inspiration really came from Doctors Without Borders, a collective of physicians who serve internationally at hotspots.
Doctors For You set out to do the same thing in India and its neighbourhood. Doctors would make themselves available in crisis situations and supplement the regular healthcare system. In India, rushing medical talent to hotspots is all the more important because of the ragged state of public healthcare.
 Cleaning up in one of the wards
Cleaning up in one of the wards
Over the years, we at Doctors For You have seen the number of natural disasters escalating. In 2019, for the first time, we responded to more than seven emergencies in just eight months. They came in rapid succession starting from Cyclone Fani in Odisha to the acute encephalitis syndrome (AES) outbreak in the district of Muzaffarpur in Bihar, the Kerala floods, Bihar floods, Assam floods, Maharashtra floods and finally the giant flood in Patna.
It was a year marked by natural disaster upon disaster and as we thought we would catch our breath and revive ourselves; we were confronted with the coronavirus pandemic in 2020.
At Doctors For You we have been engaging with governments and seeing their preparedness for calamities. It has never been enough. Some efforts are made in the form of mock drills, training exercises and post-calamity assessments. Such efforts are mostly for the record and don’t add up to much. A much larger machine needs to be in place and ready to swing into action, but as of now it simply doesn’t exist.
So, what can we do to be better prepared for crisis situations and, most dreaded of all, another pandemic, should it happen? Here are a few suggestions that come from our experience at Doctors For You:
PROMOTE SCIENTIFIC LEADERSHIP
India needs scientific leadership to look up to during a health crisis. The government’s policies and decisions should be shaped by experts with domain knowledge.
Ordinary people need both services and credible information. It can be tricky in the case of a disease about which not much may be known. Assessments keep changing and it is important that qualified people of a certain standing take the decisions that need to be taken.
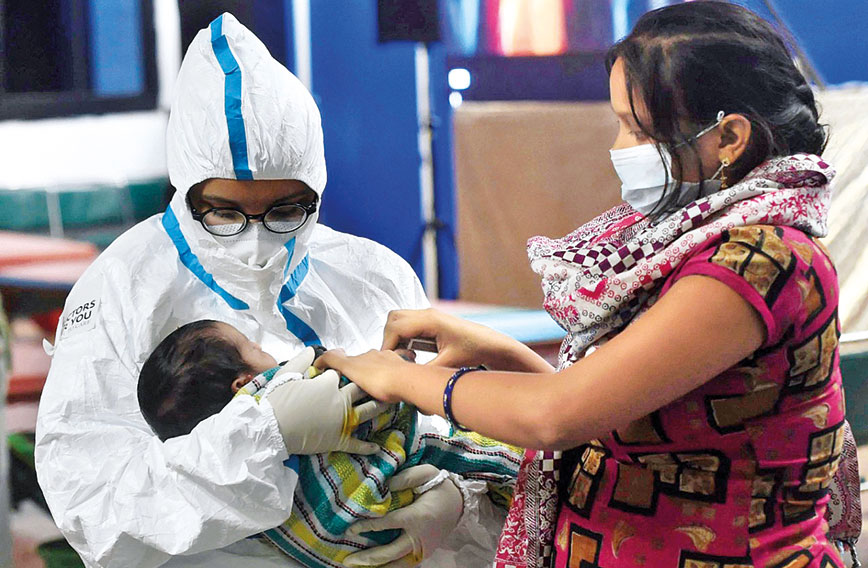 A mother with her baby at a Delhi hospital COVID ward
A mother with her baby at a Delhi hospital COVID ward
Locking down, quarantining, testing, contact tracing and even defining social norms such as mask wearing and distancing are essentially scientific decisions. Professionals should take the lead in these matters.
The pandemic in India has been addressed under the Epidemic Diseases Act of 1897 amended by an ordinance, which has now been replaced by a bill moved in the Rajya Sabha to enhance the authority of the Centre.
Having a strong central authority has its uses during a crisis. But there shouldn’t be any compromise on having scientifically qualified people in charge. On the contrary, during the pandemic we have seen bureaucrats and politicians calling the shots with a few of their chosen people from the scientific world.
The result has been that decisions and public positions have at times bordered on the absurd. For instance, long after it was apparent, community transmission of the virus was not the accepted official position.
It was similarly an embarrassing fiasco when the director of the Indian Council of Medical Research (ICMR) ordered in a letter that an Indian vaccine would have to be ready by August 15 or Independence Day. There was no way a vaccine could have been ready by then.
The National Disaster Management Authority (NDMA) originally had eight members and it currently has three. Not one of them is a public health expert. When there were eight members of the NDMA under the Congress-led UPA government, many of them were random political appointees.
Containing a pandemic requires medical doctors and scientists to show the way. High levels of scientific sophistication are needed to deal with a rapidly spreading infection.
The Secretary-General of the United Nations, Antonio Guterres, has rightly said, “Responsible leadership matters. Science matters. Cooperation matters — and misinformation kills.”
India is rich in medical and scientific talent. The country also has access to an array of respected experts in a diaspora of Indians that stretches across the globe. It is imperative that we bring this wealth of expertise together and give it an all-important role in the design and governance of healthcare systems.
There is also a great deal of learning to be done from this pandemic — here in India and in countries all over the world. Some of it has to do with treatments and the behaviour of the disease and some of it is about systems. Assimilating this learning and transforming it into a better medical response should be the work of experts.
IMPROVE THE PUBLIC HEALTH SYSTEM
There is no substitute for a robust public health system, which is accessible, affordable and run by the government. If the government healthcare system is today in a shambles, it is because of the neglect shown to it and the different degrees of bias in favour of the private sector. An imbalance has been created — it ranges from doctors’ earnings to management systems. A perception now exists that government hospitals are so bad that they can’t be trusted and are actually beyond reform.
 Beds laid out at the Commonwealth Games Stadium
Beds laid out at the Commonwealth Games Stadium
The fact is that India has a well-structured healthcare system, which goes from the PHC up to the tertiary hospital. If it were made to work better, it would deliver results like it once used to. States like Tamil Nadu and Kerala that invest in their public health systems reap the benefits. They have done better than other states during the pandemic.
We often hear that doctors don’t want to serve in the government system and take up difficult assignments. The impression is that they are only interested in making money. The reality is more nuanced. At Doctors For You we have a long list of doctors and paramedical staff who are only too happy to take up challenges. They often risk their lives. What they need is motivation and a sense of purpose.
When I landed in Delhi in the middle of coronavirus cases spiking, I got a desperate call from a private sector company asking Doctors For You to set up a hospital for their staff and family members. I asked why they needed this when all the big corporate hospitals were empanelled with the company. The answer was that these hospitals weren’t taking in the company’s patients.
Of course, government hospitals are also known to have turned away patients. But having a strong and resilient public health system is the foundation for an effective emergency response. If systems are weak even during normal times, it is foolish to expect even an optimal response during a mega crisis like a pandemic such as the one we are experiencing.
The government needs to set up a special fund for pandemics and other medical emergencies. As it is, the healthcare system is underfunded. Putting aside financial resources for crises will spare the system having to take the additional burden.
At Doctors For You we have found that companies are eager to come forward to support public health initiatives. They would be significant contributors to a special fund. Or there could be a small levy to raise funds for healthcare in the way a levy is used to raise funds for education. A levy would go a long way in raising the sizable funds required.
An alert health system with enough infrastructural facilities, equipment and skilled manpower is a prerequisite to mounting an effective crisis response. For a health system it is vital to quickly test, trace, isolate, treat and increase additional bed capacity in response to an emerging infectious disease outbreak.
 In action mode: A Doctors For You team at the Commonwealth Games Stadium
In action mode: A Doctors For You team at the Commonwealth Games Stadium
CELEBRATE THE NGO SECTOR
Such are the deficits in public healthcare in India that a giant national effort is needed. The voluntary sector has to be an important part of such an effort. Many deliverables become possible with the spirit of voluntarism. Doctors For You is an example of what a non-government organisation (NGO) can do.
There are several small hospitals in the voluntary sector. They are serving communities that would otherwise get no healthcare at all. Similarly, there are a few hundred rural surgeons with excellent degrees who forgo lucrative practices to work in rural areas.
These are great examples of the values and the spirit of service traditionally associated with medicine as a profession and not just as a business with the goal of making money.
A public healthcare system needs to be nourished with such values. Certainly, for it to work well, doctors have to be paid good salaries and given congenial conditions to work in. The management of government facilities has to serve the needs and aspirations of people employed in them. But, finally, it is the spirit of public service that has to be engendered.
An important aspect of improving public health is bringing about behavioural changes in the population at large. People with communication skills in advertising agencies can help shape effective messaging in the mass media. But the government needs socially-driven people in NGOs to go that last mile. It can’t do it on its own. NGOs have committed foot soldiers to take healthcare messages into people’s homes.
In the voluntary sector, don’t forget donors. During this pandemic the private sector has repeatedly come forward with funds. If public healthcare were to be put in mission mode, the private sector could play an important role in providing money, technology and managerial inputs.
 DFY is working in three hospitals in Bengaluru
DFY is working in three hospitals in Bengaluru
BE SUSTAINABLE
We have a consumption-driven model of growth. We need to be more Gandhian in our values. Our economic policies can’t be seen as divorced from the issues of environment and people. In fact, it should be a national objective to reduce our footprint on the planet and encourage the young to live more sustainably.
Viruses are emerging from the destruction of natural resources. The felling of forests and loss of biodiversity are ruining the balance in nature. In terms of the planet as a whole, this has its own implications. But there is enough evidence to suggest that environmentally sensitive policies translate into a better quality of life. How India manages its rivers and forests and deals with pollution will be crucial to public health. The record right now is a dismal one and has to improve.
Dr Ravikant Singh is the founder of Doctors For You. www.doctorsforyou.org
Comments
-

Umakant Shetkar - Nov. 26, 2020, 12:33 p.m.
Doctors For You is a novel philanthropic organization. In our present red tape ridden system how did DYF overcome hurdles? Many healthcare professionals like me are hesitant in organising such work. We need to learn from you.
-

Mallika - Nov. 25, 2020, 4:44 p.m.
We salute you and your tribe.
-

Sanjiv Navangul - Nov. 24, 2020, 8:45 p.m.
I have known Dr Ravikant for at least five years now. He is an outstanding person of great merit. Certainly he is the kind person who deserves the Padmashri. I worked closely with him on multi-drug resistant tuberculosis and he left a lasting impression. God bless him.



