
Dr Anoop Misra: ‘The health system is not ready for the increase in non-communicable diseases’
Move more, eat right, build those muscles
Civil Society News, New Delhi
THE COVID-19 pandemic has been the focus of the world’s attention. But is this crisis just about a new virus and the problems it is causing? Or are there larger issues involved here of unsustainable lifestyles and global warming?
Could it be that other diseases, rising silently, are intersecting with the pandemic? Perhaps there are several pandemics and epidemics that are now converging.
Topping the list of concerns are obesity and diabetes. An increasingly sedentary world is plagued by both. For India, with its inadequate public awareness, shaky healthcare system and rising incomes, the problem with these non-communicable lifestyle diseases is complex.
A major concern is the connection between non-communicable diseases and infectious diseases. Take, for instance, COVID-19 and diabetes and hypertension. Or tuberculosis and diabetes.
To walk us through this difficult terrain, we spoke to Dr Anoop Misra, chairman of the Fortis-C-DOC Centre of Excellence for Diabetes, Metabolic Diseases and Endocrinology.
In his current avatar, Dr Misra works for the private sector, but he has a distinguished record in the public sector as well — having spent long years at the All-India Institute of Medical Sciences (AIIMS) in Delhi. We bring you an abridged and edited version of an extensive interview:
Q: Dr Misra, you have said that sedentarism is a pandemic. What exactly do you mean? Is it that global lifestyles with mechanization and automation have resulted in people moving less?
Absolutely. Of course, it is a pandemic, no doubt about it. The worldwide increase in sedentarism is very well known. India is more affected by this phenomenon. People in the Western world tend to be active in their daily lives and exercise more because of the parks, open spaces and easy availability of exercise facilities.
Q: Would you say that diabetes and obesity, that have a clear connection to sedentarism, should also be seen as pandemics in which India is particularly affected?
Agree. Diabetes, the way it is growing, is astonishing. We knew 20 years back that it would go up. Unfortunately, whatever is being done is not good enough. Obesity, too, is going up and up and it takes more diseases along with it. Hypertension, heart disease, fatty liver and even cancers are going up because of obesity. It is in epidemic proportions in India. Far from reaching a plateau, we are on an ascending limb of the curve.
Q: And unless we see it as an epidemic, we’re not going to be able to deal with it on that scale.
Oh yes, absolutely. The warning about this happened some 10-15 years earlier. The curve is going up and not likely to flatten in the next decade. It will affect the health of the nation and our economy in a major manner.
Q: Are obesity and diabetes only urban phenomena? Rich people’s diseases?
It is a very good question. Some 15 years ago, we used to say this is a rich people’s disease and predominantly urban. But the scenario has changed markedly. People across economic strata suffer from it, including the poor. It is going from urban to suburban and to rural areas. The incidence has been doubling in rural areas though they haven’t caught up with cities as yet.
Q: You have worked for long in government facilities and now you are in the private sector. What is the impact obesity and diabetes on this scale are having on the public healthcare system? Do you think a redesign of the public healthcare system is now overdue?
That’s a very important and complicated question because I have seen public health systems for 40 years, right from the time when as students we used to go to villages in Haryana. At that time there would be a small, two-room OPD centre with some basic drugs. Our wonder drug at that time was a simple injection of penicillin (no other antibiotic was available!).
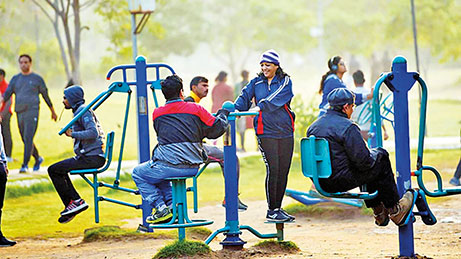 |
| Outdoor gyms make a difference |
Many improvements have been made since then. There are efficient ASHA workers at the village level and we have a much better equipped healthcare system today. There is no question about it. But the system is not prepared for the huge increase in non-communicable diseases (NCDs).
The human resources at the primary level and even at the secondary level are not equipped to deal with this surge. They are not trained to deal with NCDs in an effective manner. Just giving a tablet to somebody who has diabetes is not enough. Comprehensive advice, management of multiple comorbid diseases and careful regular follow-ups are needed. If left uncontrolled, diabetes may lead to a heart attack, stroke, kidney failure, foot infections.
Just take the example of foot infections. We often see people coming from villages with foot infections and with gangrene setting in. They have been walking barefoot. The basic health advice, to avoid walking barefoot, is not given to them and appropriate initial treatment is not given.
As a result, the foot infection rapidly becomes complicated and sometimes amputation has to be done. Diabetes is the number two cause of amputation in India, the first being accidents. Diabetes is also the leading cause of blindness and an important cause of renal failure in the country.
What we need to do is to strengthen primary healthcare. This is very important. If you go to some of the primary health centres there are persistent problems. The drugs are not available the way they should be. The doctor is also not available. And you can’t blame doctors. I mean, people do not want to go to a small primary healthcare centre and work there because of poor infrastructure, intermittent electricity, etc.
Q: What should be done socially to deal with obesity, diabetes, sedentarism?
Lots of people have thought about this before and there is a plan in place in the government. I was a part of the National Diabetes Control Programme and aligned with that is the Heart Control Programme and a Stroke Control Programme. There are common risk factors in all these diseases like unhealthy diet, lack of exercise, smoking, alcohol, stress, pollution. And all these could be effectively tackled at the primary health centre.
The national control programmes are very detailed. But the message hasn’t gone out loud and clear to the population. They need the same enthusiasm and visibility that was given to the polio programme. Most importantly we must involve all stakeholders. So far it hasn’t happened in an adequate manner. This is the downstream pathway (towards healthcare workers and the general population) for which we haven’t done enough.
The upstream pathway requires bolstering too with clear legal and policy based interventions such as increased taxes on sweetened carbonated beverages, tobacco, and unhealthy oils. Further, taxes should be decreased for healthy fruits and vegetables.
Food labelling plays an important role. Now, I’ll give you an example from Brazil where clear labels are available on foodstuff and people know what is good for them and what is not. It has brought down the incidence of obesity. This will have an impact on diabetes and heart disease too. Regulation and awareness are both required.
Q: With specific reference to COVID-19, you have said that society needs to wake up to the co-relation between infectious diseases and sedentarism. People with diabetes, hypertension and sarcopenia have been more affected by the virus. And perfectly healthy people who got infected tended to become diabetic and experience extreme muscle weakness and other symptoms.
It is clearly a two-way pathway of COVID-19 to diabetes and diabetes to COVID-19. In our research studies, a very strong relationship of both has been shown. COVID-19 is causing diabetes in people who are predisposed to it. And patients with diabetes who have uncontrolled blood sugar are getting more severe COVID-19. We knew before COVID-19 that infections are prevalent in patients with diabetes. And that’s why even before the advent of COVID-19 vaccinations, we were vaccinating diabetes patients for pneumonia and flu.
 |
| Elite runners have very low BMI but are healthy |
But, more importantly, as far as India is concerned, we have more infection-related epidemics combining with the diabetes epidemic. For example, it is happening with tuberculosis and diabetes. This we knew again before COVID-19 — that tuberculosis is occurring more in diabetic patients and somehow, though patients with TB are not obese, they have more diabetes than individuals without TB.
India was warned about this by the World Health Organization (WHO) and there are a number of research papers on this subject. It is an important issue because the COVID-19 infection may last for a short while but TB will remain for several months, and scarring because of TB will remain throughout life. There is some data to show that whatever treatment we are throwing at TB may not be as effective in a patient with uncontrolled diabetes.
This kind of coexistence of poorly controlled diabetes as well as widespread infections (a ‘syndemic’ of TB and diabetes) in the Indian population is clearly seen during the COVID-19 pandemic. We now see more patients with uncontrolled diabetes as compared to before COVID-19. As the diabetic population grows in India, unfortunately, 60 to 70 percent of cases are uncontrolled and prone to COVID-19, other viral infections and TB.
Q: The pandemic has brought many new words and terms into popular usage. One such term is ‘cytokine storm’ which prompts the immune system to get all hyper and attack organs. COVID-19 generally leaves the body wasted. You have suggested that exercise promotes early recovery. How should it be done?
It is interesting that Indians have a higher level of cytokines than Western people even when they are healthy. If you measure C-reactive protein, interleukin-6 and other cytokines, the levels in Indians will be two to three times those of people in the West. This is also true for young people in their twenties and also for non-obese people. So we already have more inflammation in the body over which when we get COVID-19 (or any other such illness), inflammation increases multiple times, converting easily into a “cytokine storm”. In such a situation the patient’s health goes rapidly downhill.
Our muscles are also thinner than those of Western people. There are many causes. Most of us are vegetarian and hence our protein intake is not adequate. We also have a tendency to be markedly sedentary.
If someone who has less skeletal muscle (termed as sarcopenia) gets COVID-19 and is in hospital for some time, the muscles are lost fast. You could lose substantial muscle during seven to 10 days of hospitalization due to fever, widespread viral infection, cytokine storm and from being in a severe catabolic state. Building lost muscle may take consistent efforts and is a slow process. It is especially so if you have a severe infection and are on multiple drugs and steroids.
Two issues have implications for post-COVID recovery. One is muscle loss, also called “acute sarcopenia”. The other is multiple nutritional deficiencies. Besides vitamin deficiencies, protein deficiency is important for muscle strength and recovery from COVID-19.
Many other deficiencies occur after COVID-19 — calcium and magnesium deficiency, etc. Altogether, your body is weak and you have a high likelihood of developing post-COVID syndromes. You may have marked fatigue, breathlessness, brain fog, dizziness, etc. Recovery is variable but generally is longer in patients who were unfit pre-COVID and have poorly controlled diabetes and other co-morbid diseases.
For recovery, exercise combined with good nutrition is necessary. A good rehabilitation programme is required for which a nutritionist and physiotherapist should be involved. With a proper programme I can assure you most patients will recover in a short time.
Q: And resistance training would be a core part of this.
I’m a great fan of resistance training because of a study that was done in 2005 by my colleague, Dr Naval Vikram, in AIIMS when I was there. We took a small number of people and put them through supervised physical exercises twice a week. Resistance training using weights and special apparatus were done under the supervision of experts. We found these individual metabolised glucose faster and their sugar levels went down significantly compared to another group that did not do such exercises.
Many people think that for doing such exercises one has to go to the gym and be under trainers. Wrong. You just have to do five to 10 minutes of resistance training at least five times a week. And this can be done at home. The instructions can be followed by just about anybody. And this is very important for people who are above 60 years with sarcopenia. You can lift small weights at any age. Some elderly people and those with heart disease think that lifting weights is bad for the heart.
This is not true. These people can learn to do resistance training with small weights under supervision. There is a good possibility that the heart’s functioning also becomes better with such exercises. Resistance training is particularly important for women to keep their muscles fit since Indian women are markedly sarcopenic and have a low level of fitness.
 For women in particular resistance training is much needed
For women in particular resistance training is much needed
Q: What is sedentarism and how should it be defined?
There are several aspects to it. First, being able to go out and exercise, and second, which is often combined with the first, is inactivity in daily life. Sitting at a desk, lying around in bed, and reading newspapers or watching TV for prolonged periods is sedentary behaviour. Such people need to move more even if it is for five minutes every two hours.
Q: It won’t do to go for a 30-minute walk and keep sitting all day.
Both the structured walk and activity through the day are required. And if you think that you can just be a couch potato for 23 and a half hours and do half an hour of physical activity and that compensates for everything it is not going to work. In such people the benefits of physical exercise are mostly lost.
Similarly, if you consume 300 calories of junk or imbalanced food and subsequently exercise, thinking that you will burn the excess calories and be fine, you are wrong. Calories from such food will be specifically injurious to the liver, kidneys and heart. And this effect won’t be counteracted by exercise. Your active lifestyle, proper diet, outdoor physical activity and resistance exercises — all of these are important.
Q: Is it necessary that you will be fat because you are sedentary? Or can you be thin and sedentary?
Yes, that is a very interesting question. You know, if you compared the average person’s weight in the Indian population to that in the Western population (we have published several research papers on this), our weight is lower than that of white people in the US or the UK.
So we are generally not too fat, specifically if we apply Western standards of body mass index (BMI). But, internally, we have extra fat. So an Indian who is 50 years old, weighs 70 kg and is five feet 10 inches with a BMI of 22, which is not considered overweight or fat, may yet have 30-40 percent body fat, clearly in excess.
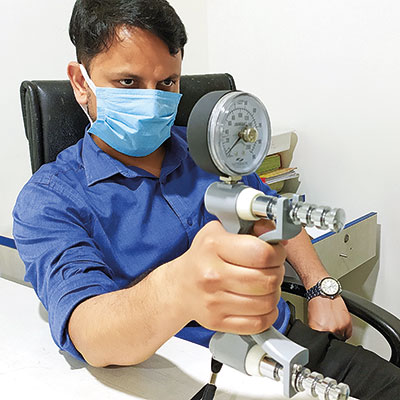 |
| Handgrip apparatus to calculate muscle power |
His abdomen and internal organs (particularly the liver) would be accumulating fat, which is bad for his metabolism. By looking at this guy and measuring his BMI, you would say he is not fat but internally he is obese. He could be termed as metabolically obese, which is having as bad a metabolism as an obese person. Without regular exercise he is certainly going to accumulate excess fat in the abdomen and internal organs. His fitness levels, already affected by internal fat, will progressively go down. Diabetes and heart disease may occur even at a young age.
On the other hand, a fat person with a BMI of 27 (obese by the Indian BMI standards) may be very active and doing all kinds of exercise and he will probably be spared many health problems as compared to a person who has a BMI of 22 but is sedentary. The reason our bodies have excess fat in almost every organ is not clear. One line of thought is that over centuries we have accumulated fat internally because that is the most effective form of energy conservation in case of famine. And our bodies continue to store fat on that ancient but still active programme.
These characteristics of high body fat, high internal fat, low muscle mass and physical unfitness are peculiar to Indians. They may not occur as much in other populations.
Q: How do I know that I am fat though I am fit-looking? Or that I am fat but actually quite fit?
You can calculate your own BMI and there are calculators on the web. In India, based on the criteria for the Indian population, if your BMI is below 23 you are normal. Between 23 and 25 you’re overweight and above 25 you’re obese. In comparison, for the West, the equivalent BMI readings are 25 and above 30 to define being overweight and obesity. These criteria for diagnosis of obesity in Indians were published by us in 2009. Now, besides being widely used in India, they are also used for Indians settled in the UK and the US.
But BMI is never a perfect measure of obesity. Because, if you look at WWF wrestlers their BMI is 35 to 40 (which is in the category of obesity) but they have huge muscles and low body fat. So if body fat is considered a definition of obesity, these people are non-obese despite high BMI. If you take long-distance runners, in particular elite marathon runners, their BMI is often below 18.5, which we can consider to be undernourished. But they are all muscle, their body fat is below 10 percent and they are extremely fit.
Hence BMI as a criterion of obesity and body fatness has fallacies. It will not tell you your body fat or abdominal fat. It will not tell you about your muscles. For that you have to go to more sophisticated instrument-based measurements.
In the research centre I am sitting in, we have many such instruments. One of them is a simple
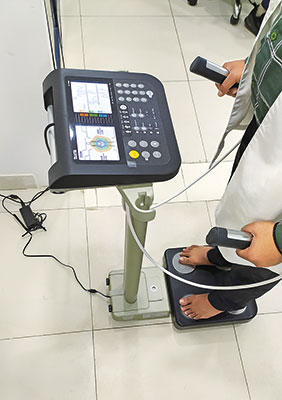 |
| A simple bioimpedance apparatus |
bioimpedance apparatus. What we see in gyms are the cheapest versions of this instrument. They are never very accurate. More sophisticated versions are more expensive and more accurate. A bioimpedance machine passes a low-grade current through you, to assess the impedance of body water. It will calculate how much body water you have and by using an inbuilt equation it will tell you your body fat. It is never accurate because it will be affected by multiple factors. For example, if you have had a couple of litres of water to drink, the reading will vary. Most accurate for measurement of fat is a dual-energy X-ray absorptiometry, called a DEXA scan, an immovable apparatus and only available in select centres.
For measurement of fitness or assessment of muscle power more expensive instruments are required. For example, we can make the person run on the treadmill and measure oxygen efficiency. It is usually meant for elite athletes and sportsmen. We can assess muscle power by using a handgrip apparatus. In a few seconds you will know how much muscle power the person has.
Q: But if I am not a world-class athlete, just an ordinary person who wants to know whether he is fat despite being fit-looking, what do I do?
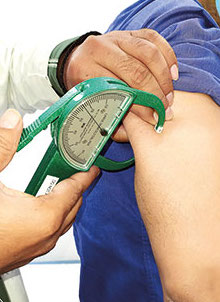 |
| The calliper can calculate body fat |
There are other very simple ways of estimating body fat. One of them is using a calliper to judge subcutaneous fat. The calliper, used in four places, can calculate body fat. The other important measurement which I must emphasize is waist circumference, which is an indirect measure of abdominal fat, a very important risk factor for heart disease. The bigger the waist the more the likelihood of heart disease, hypertension and diabetes. Normal values of waist circumference should be less than 90 cm for men and 80 cm for women. Some consider this measurement to be more important than BMI for assessing overall heart risk. These criteria for the Indian population were published by our research team.
Q: With the calliper you are basically pinching the body?
It looks small but it costs Rs 40,000. It is very accurate. Fat is measured in millimetres. It assesses how much subcutaneous fat is there in that area. It is interesting that Indians have higher subcutaneous fat than other races.
Comments
Currently there are no Comments. Be first to write a comment!



