
Araku lifeline brings maternal deaths to zero
Swapna Majumdar, Araku Valley
Surrounded by dense forests, Araku Valley in Andhra Pradesh's Visakhapatnam district is rich in biodiversity, but its people are poor. So remote are some of the tribal hamlets here that in 2011 they escaped the eye of the census.
As a result of this isolation, healthcare services do not reach people. Pregnant women cannot be taken to hospital for want of roads and transportation. The rates of maternal and infant mortality across the valley have always been depressingly high.
But signs of change are evident six years since Piramal Swasthya launched a programme called Asara to reduce maternal and neonatal deaths. Health workers have been monitoring families and telemedicine has provided access to physicians over long distances. The first results are very encouraging.
“No maternal deaths have been reported from 181 hard-to-reach hamlets in the Araku Valley since we began our programme,” says Vishal Phanse, CEO, Piramal Swasthya, the rural healthcare initiative of the Piramal Foundation.
“We went to Araku Valley to find the gaps in healthcare and plug them. We wanted to supplement the government’s efforts. To end maternal deaths, we were prepared to sit near villages, even with a palki, and rush the woman to hospital as soon as she was ready for childbirth,” he recalls with enthusiasm.
In 2011, maternal mortality in this region was 400 per 100,000 live births, nearly double the national average of 215 per 100,000 live births. Neonatal mortality was over 60 for every 1,000 live births. The national average, at that time, was around 44 per 1,000 live births.
Asara has reached out to 4,900 women over six years and helped facilitate safer childbirth. “Institutional deliveries increased from 18 percent in 2011 to 68 percent in 2017 in our project areas,” says Phanse.
Emboldened by this success Piramal Swasthya now plans to expand the programme to 1,179 habitations.
 Vans like this one get women to Piramal Swasthya’s telehealth centres
Vans like this one get women to Piramal Swasthya’s telehealth centres
Asara uses technology and feet on the ground to reach healthcare to pregnant women and babies. Telemedicine centres, linked to obstetricians and gynaecologists in hospitals, are set up and trained ANMs (Auxiliary Nurse Midwives) go village-to-village registering pregnant women, providing services at their doorstep, and taking them to the telemedicine centre and to the government hospital for their deliveries.
Piramal Swasthya had earlier been working with the government in 13,000 out of 17,000 villages in Andhra Pradesh. The experience was invaluable. It also resulted in the raising of a dedicated workforce of 4,000 paramedics and medical personnel.
“The opportunity to work with a million beneficiaries every month gave us direct access to people and data. That helps us come up with predictive analysis. So we can customise solutions district-wise and share those with the government,” explains Phanse.
“We had identified Araku as a very vulnerable place,” he says. “Although the government has a huge budget, it doesn’t have innovation in its DNA. I use our CSR budget for innovation and take it to scale. Innovation can be risky, but in Araku we succeeded. We focused on accessibility, affordability, and availability of maternal health and managed to bring down maternal deaths to zero in the last two years.”
TECH AND MEDICINE
In 2010 Piramal Swasthya launched the Asara project by carrying out a baseline survey in Araku Valley to get a picture of the challenges that lay ahead.
The survey found that the female literacy rate was just 37.28 percent — much lower than the state’s average of 59.74 percent. There was poor awareness of health issues and lack of access to healthcare facilities. Forty of the 181 villages had not been counted by the 2011 census.
Since most of the 181 hamlets chosen for the first phase of the project were remote and hard to reach, it was decided to set up telemedicine centres. In 2011 the first telemedicine centre was started in Araku mandal. In 2017 two more were set up, one in Paderu and the other in Chintapalle. Paramedics were trained to provide antenatal and postnatal care services to women at their doorstep and then link them to specialist doctors via video conferencing at the telemedicine centre.
Many lives have been saved. Take 17-year-old Chandrakala, who came to the telemedicine centre at Paderu for a routine antenatal visit. Her tests revealed she had malaria — for the second time. Dr J. Himaja, resident doctor at the telemedicine centre, got worried. Chandrakala was in her ninth month of pregnancy. She had been treated for severe anaemia and malaria just a month earlier when she had come for her third antenatal visit.
At that time, the team at the centre had rushed Chandrakala to the district hospital in Visakhapatnam, 96 km away, and ensured she was given a blood transfusion to boost her haemoglobin count. They had pooled their own money to pay for her hospitalisation, realising it would be fatal to let the impoverished Chandrakala return to her village without treatment.
So, Dr Himaja knew she was a high-risk case. Within minutes, Dr Rajyalaxmi, an empanelled senior gynaecologist based in Piramal Swasthya’s headquarters in Hyderabad, was contacted through video-conferencing and apprised of Chandrakala’s condition. Since records of all patients of the telemedicine centre are uploaded, it did not take Dr Rajyalakmi much time to pull out Chandrakala’s medical history.
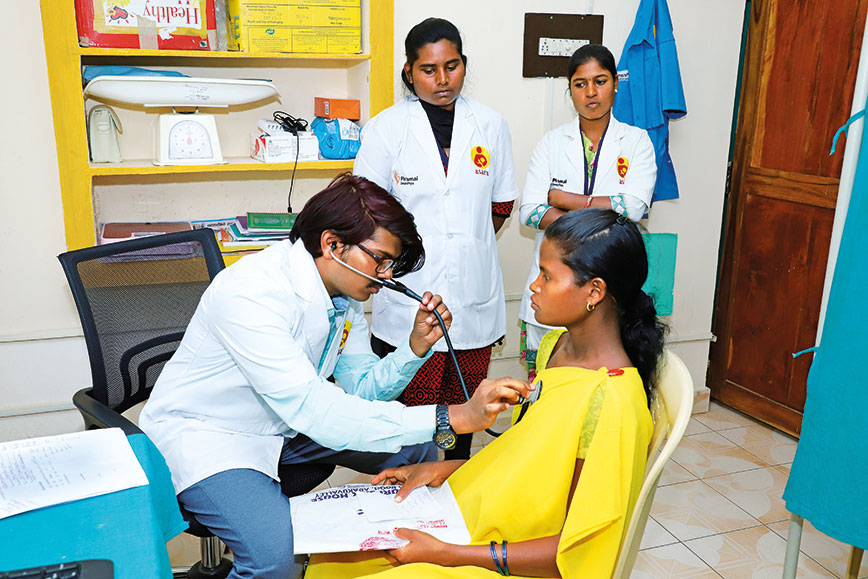
 Dr J. Himaja seeks advice via video conferencing on Chandrakala’s (in yellow sari) case
Dr J. Himaja seeks advice via video conferencing on Chandrakala’s (in yellow sari) case
She asked Chandrakala, sitting alongside Dr Himaja in front of the monitor, a few questions. But Chandrakala, who belongs to the Kondadora tribe categorised as a particularly vulnerable tribal group by the government, could not understand Telugu. She speaks only a local tribal dialect and everything was translated.
Dr Rajyalaxmi advised Dr Himaja to take Chandrakala to the hospital immediately. “Since she doesn’t understand Telugu, you must accompany her. She will be reluctant to stay in the hospital as she may feel it is unnecessary. You must ensure she gets a blood transfusion. Counsel her husband and don’t leave her alone,” urged Dr Rajyalaxmi.
It was this speedy action and personalised care that ensured Chandrakala and her 18-year-old husband welcomed their first child without further complications.
ROLE OF ANM
It is Asara’s trained ANMs who connect the women to the telemedicine centre. Since many hamlets do not have proper roads, a male colleague takes the ANM on a motorcycle across rough terrain. Often the ANM has to complete the last few kilometres on foot.
Once they reach a village, the ANMs make a list of all the pregnant women and newborn babies. The pregnant women are registered and each one is given a unique identification number after recording weight, height, and blood pressure as part of the initial examination. Samples for blood and urine are collected for tests.
Anaemia and eclampsia (high blood pressure with seizures) are the most common prenatal complications prevalent among pregnant tribal women in the district. Therefore, the outreach service includes comprehensive risk-profiling of pregnant women and health-counselling. Free calcium and iron folic acid tablets are also given.
The next day, the telemedicine centre’s jeep is sent to pick up all the registered pregnant women from the point closest to their village and bring them to the centre, where a staff nurse notes down a more detailed history. Once the data is collated it is digitised. These electronic health records help keep track of the health of the pregnant women and newborn babies. They are also shared with the government hospital when a pregnant woman arrives for her delivery.
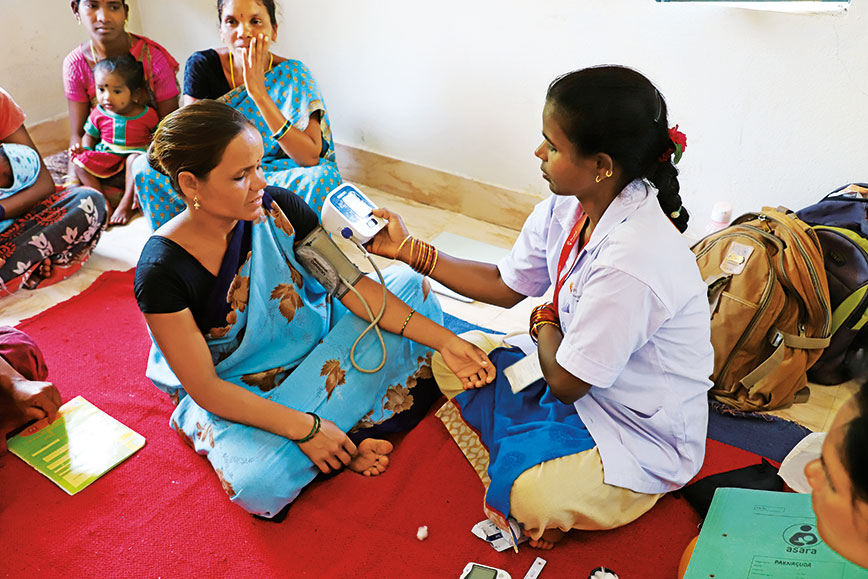 B. Pramilla, an Asara ANM, checks the blood pressure of a pregnant woman
B. Pramilla, an Asara ANM, checks the blood pressure of a pregnant woman
The data comes in handy when a patient is brought to the telemedicine centre for routine checkups, or connected through video-conferencing to a specialist gynaecologist based in Hyderabad for advice. At the centre, pregnant women are given calcium and iron and folic tablets. Lunch is also served to all pregnant women and lactating mothers. Then they are dropped back to their villages.
The Asara programme, which runs on an annual budget of Rs 50 lakhs for each telemedicine centre, spends an average of Rs 650 on each registered patient.
FRONTLINE WORKERS
The ANMs traverse forests and steep hills, cross streams and walk several kilometres of undulating roads to ensure no woman dies while giving birth. Each of the four ANMs on field duty earns Rs 15,000 per month and has been given the responsibility of reaching out to 45 villages every month.
When P. Champa, an ANM, has to go to Pedagaruvu, a small village of 43 families, she sets out from the telemedicine centre before 8 am, riding pillion on a motorcycle. She is dropped about 15 km from the village and does the rest of the distance on foot.
After she arrives in the village she spends the next few hours checking up all the pregnant women who have registered for the Asara programme. On the basis of this check-up their records are updated.
After making sure no one has been left out, Champa walks to the next village. “It is even tougher the day I go to Nanda village, since it is 36 km away from the telemedicine centre. I have to walk for almost two hours up hilly terrain. I have three registered pregnant women there. Also, one woman just delivered in March and her postnatal care has to be ensured. I have to check that she is breastfeeding her child and has not forgotten why it is important,” says Champa.
The emphasis on informing pregnant women and new mothers of the benefits of breast milk is crucial. Superstitions abound among tribal women that breastfeeding leads to indigestion and harms the child. The hard work put in by Champa and the other ANMs is getting the message across. Assessment figures indicate that 50 percent of newborns are breastfed within half an hour after birth, and 98 percent of mothers continued to give colostrum milk to their children for the first few days after birth.
Building this trust has taken time and persistence. It has meant changing mindsets. B. Pramilla, an Asara ANM, is six months pregnant. Yet she braves the heat and walks through a long winding road to Ranginigudda village to check out K. Laxmi.
Laxmi, 28, gave birth to her second child in March this year. When Pramilla asks her about her baby, Laxmi has no qualms in handing him over to her.
“I am uneducated but I know that had Pramilla not been there, my baby and I may not have been alive,” says Laxmi.
She is right. Pramilla recognised signs of pre-eclampsia — persistent oedema on Laxmi’s feet and traces of albumin, bile salts, and bile pigments in her urine, also indicating the possibility of hepatitis.
“Besides, what made Laxmi a high-risk case was that in her last pregnancy, she had gestational hypertension and suffered loss of consciousness during childbirth,” says Pramilla.
Not wanting to exacerbate the risk, Laxmi was taken to the telemedicine centre where Dr P. Shamukha Reddy, the resident doctor, persuaded her to undergo tests to reconfirm Pramilla’s diagnosis. Once lab tests confirmed her chances of developing pre-eclampsia and possible eclampsia at the time of delivery, Laxmi was advised to get admitted to the area hospital immediately.
Instead, Laxmi went home saying she would come the next day. But the same night she went into labour and called Pramilla. “We reached there just in time and facilitated her admission to the hospital. Had we been late, there could have been complications. Thankfully, both the mother and baby are safe and healthy,” says Pramilla.
Champa, like Pramilla, acts promptly when she receives distress calls by pregnant women. “Some months ago I got a call at 1 am from the family of a pregnant woman when she went into labour. As she suffered from epilepsy, we had to be really quick in getting her to the hospital. I called the telemedicine centre immediately and went to pick her up. Since she was in Sabaka, one of the hard-to-reach villages, the jeep had to stop at the closest point. We then walked up to her house and brought her down on a bed. We rushed her to the government area hospital where she had a safe delivery. I feel really happy that we saved her life,” says Champa.
 Dr P. Shamukha Reddy examines a patient at the Araku telemedicine centre
Dr P. Shamukha Reddy examines a patient at the Araku telemedicine centre
Fundamental to the success of Asara is the rigorous process the ANMs follow from the time a pregnant woman is registered. “Our ANMs support the women and children right through their pregnancy, childbirth and neonatal period. Each woman registered with Asara receives four antenatal checkups and one prenatal checkup. High-risk pregnancies are identified at the time of registration and provided appropriate medical advice and treatment. Periodic checkups till the time of delivery are critical for reducing maternal deaths,” points out Swarnalatha Tirlupathi, Asara’s programme manager.
COOPERATION AND COORDINATION
The strategy to forge a working relationship with the ASHAs or Accredited Social Health Activists and anganwadi workers has also helped the Asara programme, explains Ramanujam Mantraratnam, the operations manager of the Asara programme in Araku Valley.
Sumitra Dalpati, an anganwadi worker in Pakmaguda village, not only helps the Asara ANMs identify pregnant women but also provides them a list of their names and contact details.
“The government-appointed ANM is supposed to come every third Wednesday of the month. Sometimes she doesn’t come. But Champa arrives on the 17th of the month and goes from house-to-house to check on all the pregnant women. The government ANM does not have the time to do that because she has to go to so many other villages,” says Sumitra.
This dedication is what motivated 23-year-old Shakuntala, pregnant with her first child, to register with Asara. “I heard about the programme from other women in the village. I am not educated but I understood that this would benefit me and my child,” says Shakuntala.
Twenty-one-year old Renuka, on the other hand, has studied till Class 7. She comes with her husband Nageshwar Rao to the anganwadi centre where Champa, the ANM from Asara, is carrying out routine ANC checkups.
Nageshwar supports Renuka’s decision to register with Asara. “This is our first child. We were not aware of what needs to be done. After Renuka registered, she told me about the health advantages under this programme and convinced me. After that, if needed, I go with her for the checkups,” said Rao.
ASHAs also readily accompany the Asara ANMs when they take pregnant women to hospital for deliveries. One reason for this camaraderie could be that the project ensures the ASHAs get an incentive for bringing women for institutional deliveries. However, the ASHAs say that the Asara programme has made their work easier and both are able to work in tandem.
Muthuamma, an ASHA who has been working in Kaguvalasa village for the last 20 years, says that when she met Pramilla, the Asara ANM, and was informed about the programme, she did not feel threatened. “They support us in making sure no woman is left behind. Since the government hospital is really far away, it is difficult for women to go there. Pramilla takes the women to the hospital free of cost. I accompany them. So we work together,” says Muthuamma.
 Women listen to advice on healthy foods at the nutrition hub
Women listen to advice on healthy foods at the nutrition hub
NUTRITION HUB
It was while working with the community that the Asara ANMs found many women were anaemic. In 2017, after thorough research, Piramal Swasthya started a nutrition hub to improve local knowledge and practices on nutrition during pregnancy and lactation as well as to ensure children under five years received the right nutrition.
The hub, located in Paderu, houses a solar dryer and teaches the women how to preserve seasonal and local vegetables to ensure food security during the lean season. Women learn to make nutritious meals from homegrown vegetables and how to preserve dehydrated nutrient-rich foods to combat anaemia and undernutrition.
The Asara programme is emerging as a model to end preventable maternal death among tribal women. But challenges still exist. Apart from the tough terrain, Asara is grappling with issues such as poor access to safe drinking water, basic sanitation, and hygiene. The lack of these amenities poses health risks for pregnant women and lactating mothers.
Piramal Swasthya is keen to scale up its project and address the interplay between clean water, sanitation, and maternal health. With the experience it has gained it should be able to end maternal deaths, not just in Araku but in all the 11 mandals in the tribal belt of Visakhapatnam.
-----------------------------
‘We will take Araku model to all tribals’
 Vishal Phanse, CEO of Piramal Swasthya, has an ambitious agenda: to reduce maternal mortality among tribal communities in India by using the Araku project as a model. His office in Hyderabad has a whiteboard with scrawls and squiggles — perhaps it’s a roadmap to spread better maternal health across India. Piramal Swasthya is working closely with the government and finetuning its strategies to achieve this.
Vishal Phanse, CEO of Piramal Swasthya, has an ambitious agenda: to reduce maternal mortality among tribal communities in India by using the Araku project as a model. His office in Hyderabad has a whiteboard with scrawls and squiggles — perhaps it’s a roadmap to spread better maternal health across India. Piramal Swasthya is working closely with the government and finetuning its strategies to achieve this.
Extracts from an interview:
Why did Piramal Swasthya decide to focus on maternal and infant health?
Our mandate is to transform the health ecosystem, which we can do through partnerships. We studied the primary healthcare space in India and found that though there are many good NGOs working in this space, nobody had the ambition to scale beyond a district for various reasons.
We believe that to transform India we have to scale up. Since we were working on health issues in 13,000 out of 17,000 villages in Andhra Pradesh, we had the advantage of having 4,000 paramedics and medical personnel in the field. The opportunity to work with a million beneficiaries every month gave us direct access to people and data. That helped us come up with predictive analysis. So we can customise solutions district-wise and share those with the government.
Has there been any change in strategy along the way?
We wanted to focus on changing health-seeking behaviour. So our strategy was to stay with the community and learn from them. Two years ago we realised that without a nutrition intervention in place, our initiative would not have a sustainable impact. This need came from the community. So the nutrition hub came up as an additional component to our strategy. Its use of locally available, culturally accepted foods and diet gives a push to holistic, indigenous, self-sustainable solutions.
We believe that our model will have significant impact on the overall health indicators of Visakhapatnam district and thereby on Andhra Pradesh. I want to use the Araku model for all the tribal communities in the country. They comprise 10 per cent of India’s population. This means we have 120 million tribal people. Their maternal mortality rate is close to three and a half times the national figures. So we have directed all our efforts towards achieving the Sustainable Development Goals (SDGs) both for maternal mortality and neonatal mortality.
Will you be using the Asara model to upscale at the national level?
Absolutely. About 60 percent of the population in Visakhapatnam district is tribal. We thought if this works in 181 villages, it should work in 1,200 villages with the nutrition component added. We are also evolving a better telemedicine strategy not just for Araku but for the whole country since we are advisors to the Ministry of Health and Family Welfare on rolling out telemedicine technology.
Will you also be tackling issues like safe drinking water, basic sanitation and hygiene?
We haven’t focused on these social determinants so far. But we are good at learning. We are trying to work on a model within Araku. One of the plans I have is of creating a pool of health fellows who will help in coming up with solutions. We are hoping to launch this in 2019. We have also just started working with adolescent girls, educating them about all these issues. We are thinking through these issues and then putting a plan in place.
Are you happy with the Araku model?
We are Niti Aayog’s knowledge partner in 100 of its aspirational districts. This is not only because we now serve one million people in 16 states but primarily because of Araku. So not only am I happy, I love the work.
Comments
-

vivek sharma - Feb. 13, 2020, 10:41 a.m.
great work . but why NGO has to do all this ? , people hired by govt to which they will give pension should be made accountable.



