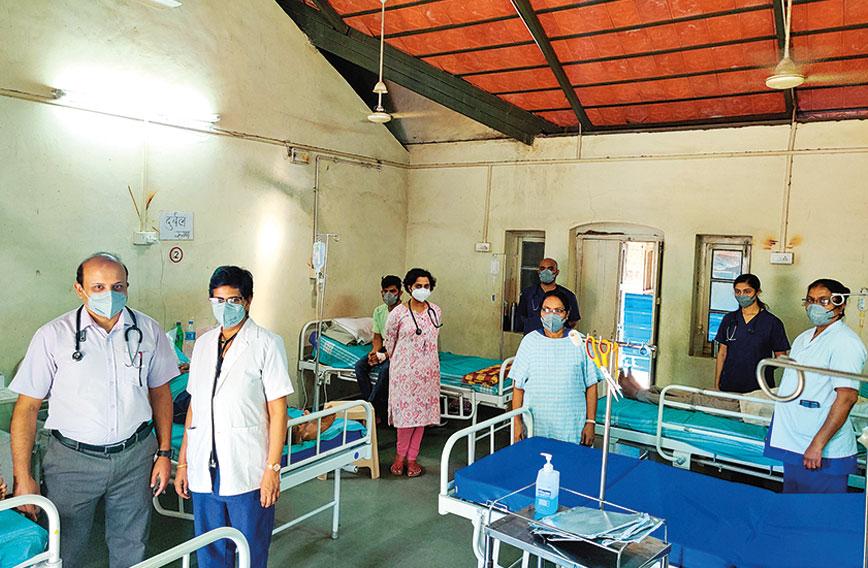
Dr Deepak Singh and Dr Ashita Singh at the Chinchpada Christian Hospital
Blessed is the rural hospital
Civil Society News, Gurugram
IT’s a dreary morning in May. The news from all over the country is of deaths, cremations and patients trying to find beds in hospitals. In sharp contrast, at Chinchpada, a small village in Maharashtra, a thanksgiving is being held.
The occasion is the installation of an oxygen plant at the Chinchpada Christian Hospital, which will greatly enhance its ability to provide treatment to COVID-19 patients of the area.
We are invited to the inauguration and rush through our morning in Gurugram to show up at Chinchpada on Zoom at 7.55 am sharp. A distance of 1,076 km separates us, but technology and the virus have brought villages and cities closer than ever before.
Also Read - Kerala model: When the frontline is backbone
Music, prayers and balloons set the mood for the occasion. The inauguration is presided over (also on Zoom) by the District Collector, Rajendra Bharud. He is famous for having ensured that Nandurbar district, in which Chinchpada is located, hasn’t suffered from a shortage of oxygen. He foresaw what was coming and acted in good time.
Bharud is himself a Bhil tribal from the area. He was raised by his mother in poverty, but went on to study medicine and then join the Indian Administrative Service (IAS). He is brisk and businesslike, but without the airs of officialdom or so it seems to us. From the few minutes that we observe him, we get the feeling his heart is invested here in this backward region.
As the brutal second wave of the pandemic spreads in rural areas, and fear mounts of a third wave, there is growing concern over how people in far-off villages like Chinchpada will find treatment. Also, if the virus continues to go unchecked in villages, cities can hardly hope to be safe from further rounds of infection. Everyone is finally connected.
The timing of surges will vary from one part of the country to another distant part. We can already see that happening as we talk to physicians in different locations. What is that going to mean in terms of transmission of the virus and mutations? No one really knows.
The situation is grim and full of foreboding. Dealing with a pandemic like this one requires an extensive and effective healthcare system that creates awareness, treats patients quickly and vaccinates people where they live.
But years of neglect by successive governments have resulted in the Indian public healthcare system not functioning in large swathes of the country. Now, with the pandemic here, there is no time to set things right.
The whole system can't be improved overnight, but it can be energized in parts. Even in rural areas people will find facilities in the government system that do work, particularly in states like Tamil Nadu and Kerala where investments have been made over time.
Then there will also be facilities in the voluntary sector, such as the Chinchpada Christian Hospital, with good medical professionals who have moved far out of big cities to provide healthcare to people in remote locations.
 An oxygen plant is inaugurated and staff of the Chinchpada Christian Hospital line up for pictures
An oxygen plant is inaugurated and staff of the Chinchpada Christian Hospital line up for pictures
The pandemic, for all the stress it is causing, is also the time to begin envisioning a better system by learning from what works during this crisis. Perhaps then, going forward, it will be possible to serve the healthcare requirements of a billion people in everyday conditions and during emergencies. There is a growing burden of diseases that have to be dealt with and this certainly won’t be the last virus that will visit us.
With its 50 beds and a team of well-trained doctors and nurses, the Chinchpada Christian Hospital is really a model of the values and standards that should imbue public healthcare. The hospital is affordable and accessible and provides high quality medical treatment. It is driven by the spirit of service.
It is also closely linked to the local community, which in the case of Chinchpada and its neighbourhood consists mostly of tribal people with limited means. It has taken healthcare out of the hospital and into homes and villages, making primary care an everyday thing for which people are as much responsible as the doctors who treat them.
Over time, the hospital has engendered local confidence in its services. A patient, no matter how poor, can walk in, ask for a doctor and actually find one. As a result, from the first wave itself people infected with the virus have turned to it in growing numbers.
The hospital functions as a trust under the larger umbrella of the Emmanuel Hospital Association. The oxygen plant has been funded with a donation of `28 lakh made by Azim Premji Philanthropic Initiatives.
But it is not on donations alone that the hospital survives. It has found its own financial viability by balancing user charges and costs, particularly by purchasing generics and moderating what its doctors get paid.

Dr Deepak Singh and Dr Ashita Singh at the Chinchpada Christian Hospital. It has a modest exterior but patients receive advanced treatment
The OPD charge is a modest `20. A stay of four to five days in the hospital works out to an average cost of Rs 5,600. The hospital had 25,000 patients last year of which 4,000 were in-patients.
Established by missionaries in 1942, the Chinchpada Christian Hospital has had ups and downs. Its current reputation has been built since 2014 by Dr Deepak Singh, a paediatric surgeon, and Dr Ashita Singh, a physician.
They are husband and wife with advanced degrees from the Christian Medical College in Vellore and Ludhiana. The team consists of the two of them as surgeon and physician, an anaesthetist, a dentist and 25 nurses and medical attendants.
GROWING DEMAND
With the pandemic, demands on the hospital’s facilities have multiplied. Not least among them is the requirement for more oxygen for which the oxygen plant was needed, especially if a third wave of the virus were to happen.
“We now have enough oxygen for 67 patients at a time. This includes 10 ICU beds. We hope the third wave doesn’t come but we are preparing for it with another 10 ICU beds and 30 oxygen beds,” says Dr Deepak Singh.
“The oxygen requirement in the district went up very significantly during the second wave,” he explains. “Even our small hospital went from using 10 cylinders a day to 26 to 28 jumbo cylinders in a day to provide high-flow oxygen to 57 patients at the peak.”
During the surge, the cost of a cylinder went up from Rs 12,500 to Rs 20,000. The charge for refilling a cylinder went from Rs 300 per cylinder to Rs 500 and then Rs 1,000 in the second week of April. Transporting cylinders from Surat meant an additional cost of Rs 4,000.
Dr Singh recalls how difficult it was to balance demand and supply. A moderately infected patient needed between five and 10 litres per minute of oxygen. A severely affected patient needed 10 to 15 litres per minute.
“We rationed oxygen by keeping lower targets of oxygen saturation between 92 and 94 percent. This allowed us to give oxygen to more people at lower rates of flow,” he says.
Now the new oxygen plant has been connected to the cylinder manifold. If at any time the pressure in the plant drops, 35 reserve cylinders take over.
PRIMARY CARE
The pandemic has underlined the need for taking healthcare to the doorsteps of patients so that they don’t end up flooding hospitals.
The Chinchpada hospital provides primary services, but it is really a secondary level facility that does general surgeries, handles deliveries and treats a whole lot of diseases.
It coordinates with the local government-run primary health centre and district centre. They connect with each other as the need arises.
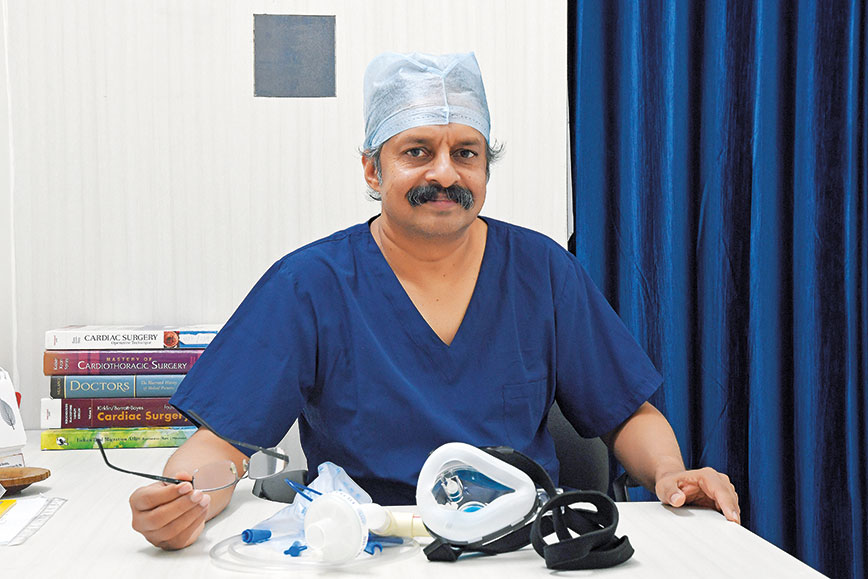 Dr Sanjeeth Peter and his improved oxygen mask: ‘A heart surgeon is essentially a plumber’
Dr Sanjeeth Peter and his improved oxygen mask: ‘A heart surgeon is essentially a plumber’
India’s healthcare system is actually designed to have a structure that begins with primary and community centres, above which come district hospitals and then tertiary facilities.
The problem is that the system doesn’t function in the absence of investments in people and infrastructure. There is confused policymaking and lack of administrative will. A perfectly good design for a system lies in disuse.
One piece of learning from the pandemic is that voluntary initiatives should be better integrated with the government system — both to bolster it and to raise standards.
LAST-MILE DELIVERY
Dr Pavitra Mohan in Udaipur, in Rajasthan, says that there is no substitute for a primary care approach which is close to communities and built with their participation. It should be evidence-based and address social realities, he says.
Dr Mohan, a paediatrician, and his colleagues set up Basic Healthcare Services (BHS), a non-governmental organization, eight years ago because they felt there was a problem with delivery of health services to last-mile communities.
Between 2005 and 2012 there were several policy changes taking place at the national level and in the states with which they were involved, but the benefits were not really reaching people.
They set out to know more about it in a hands-on way by setting up, under BHS, six AMRIT Clinics in the catchment of two or three panchayats with a population of 12,000 to 15,000 each. These are all between 20 km and 70 km from Udaipur city, where Dr Mohan is based.
There has been interesting learning from their initiative. For instance, there is the realization that it is difficult for doctors to live and work in last-mile communities.
 |
| Dr Pavitra Mohan |
“Doctors are required for clinical care, but they are not best suited to take care of the many conditions that exist. A bulk of the clinical care can be delivered by nurses who are from tribal communities,” he says.
The nurses have qualifications as General Nurse and Midwife (GNM) or Auxiliary Nurse and Midwife (ANM) or have a B.Sc. in nursing. There are also community health workers and volunteers.
In this way the doctor at an AMRIT Clinic needs to visit the clinic once a week and for the rest of the time is available 24x7 for consultation, leaving the nurse to feel empowered and responsible for patients.
“There is a set of diagnostics and the most commonly used drugs — about 280 to 300 of them — which are available within the clinic. We use technology judiciously for diagnostics and wherever required for teleconsultation, etc. But we believe that technology can only enable and not replace the human touch and these skills still require skilled and empathetic providers at the front end,” explains Dr Mohan.
AMRIT Clinics are located in community-owned buildings taken on lease by BHS. There is a tie-up with a hospital for cases which require a higher level of attention. “Referrals are escorted and supported,” says Dr Mohan.
BHS also runs a PHC in partnership with the government of Rajasthan, which covers a population of 25,000 in order to ‘integrate’ the learning at the AMRIT Clinics with what the system offers.
Says Dr Mohan: “We realized that there is a huge untapped potential within the public system. It can do wonders with some support and strengthening.”
“We believe that nurses, when supported and enabled with technology and training, can deliver the bulk of care. Social beliefs also change. But it does require more patience than one often has for influencing behaviour,” he says.
It is similarly important that healthcare be seen in conjunction with employment. To this end, BHS works closely with Aajeevika Bureau, an NGO that addresses the needs of workers in the unorganized sector, in particular those given to migration.
MIDWIVES IN CHARGE
Dr Sharad Iyengar, paediatrician and community medicine specialist, similarly believes that there is scope to improve the system. It can be reenergized by engaging with it. Solutions lie in breaking with stereotypes.
Dr Iyengar is the chief executive of ARTH, which stands for action, research and training for health. Like Dr Mohan, he is based in Udaipur and ARTH’s work is also in southern Rajasthan. In the past, Dr Iyengar and Dr Mohan have worked together though currently their outfits are distinct from each other.
 |
| Dr Sharad Iyengar |
Dr Iyengar’s focus has been on preventing maternal deaths during delivery. He has trained nurse-midwives to play leadership roles during deliveries by undertaking life-saving medical procedures. They also counsel women on their reproductive and sexual health.
Dr Iyengar was prompted to start ARTH when a 1998 survey showed that most deliveries in Rajasthan were at home and deaths were common.
He began by training just two nurse-midwives. But over the years there have been 14,587 deliveries handled at ARTH’s two rural centres and 93 percent of them have been handled successfully by midwives. The remaining seven percent were referred to hospitals for complications which were identified at the clinics.
Nurse-midwives are in residence at ARTH’s centres with their families and are available round the clock. In the role given to them, they are meant to substantially replace doctors who are available on call for emergencies.
“Women receive care as per World Health Organization (WHO) and government guidelines,” says Dr Iyengar. “It is proven that midwives with training can handle 80 percent of maternal and newborn complications.”
The ARTH model takes quality care to the women who need it. The midwives receive a high level of trust within the communities with whom they engage. By empowering the midwives, ARTH helps them acquire an identity of their own and over time they play leadership roles. The scientific practices they stand for become what the community begins to espouse.
A big part of the problem with reforming public healthcare is that entrenched interests, often doctors themselves, don’t want to let go, says Dr Iyengar.
But fresh thinking is needed to suit different contexts. It also brings gains when they are needed most. For instance, during the pandemic, government services have been deployed for dealing with the virus. There have been lockdowns to contend with. Pregnant women have nowhere to go for check-ups and deliveries.
“But ARTH’s centres functioned without a break during this time,” says Dr Iyengar. “Between March 2020 and March 2021, midwives attended 1,025 deliveries.”
TRUST MATTERS
Building trust in the system is key to improving it, says Dr Mohan. Training and empowering frontline workers like ASHAs is therefore important. Users need to know the system to be dependable and caring. They should be active participants in its success as well.
For Dr Mohan basic healthcare is what matters. The pandemic is proof that well-functioning primary and community health centres would have created awareness and led to the treatment of mild and moderate coronavirus cases without them having to show up at hospitals.
Some of this has happened in Rajasthan. During the pandemic it is at the PHC and community health centre levels in Rajasthan that COVID-19 awareness and treatment of mild and moderate patients is being done. But it is not enough.
“We have been advocating oxygen and concentrator supplies to PHCs. We have ensured availability at our clinics,” says Dr Mohan.
“In Rajasthan, it is doable to handle the surge of COVID-19 cases at the primary level. There are the buildings and the equipment and the staff,” says Dr Iyengar.
The problem is a long-term one of establishing competencies and conditioning the system to be sensitive and responsive when the need arises.
LOCAL AWARENESS
In the tiny village of KC Patty in Tamil Nadu, a long way from Udaipur, Dr Rajkumar Ramasamy voices similar concerns over an ill-prepared primary healthcare system and laments the problems with a top-down approach.
KC Patty is tucked away behind reserve forests in the foothills of the Western Ghats. There are tribal hamlets scattered around. Dindigul is the nearest city, some six km away. The town of Oddanchatram is 60 km away. Madurai is at a yet greater distance.
So, it is a pretty far-off place that we are looking at, but the virus has arrived and the local people are confused. They don’t know what is happening to them. It is especially daunting if health officials turn up in personal protective equipment (PPE) suits.
KC Patty’s problems are an example of the complexity of delivering healthcare in India. The village and its neighbourhood has seen its own surges in the virus, which has arrived through traders coming to KC Patty and local people travelling out to markets. Townspeople have also been buying land in the area and during the pandemic have tried relocating to escape the virus. Instead, they have brought it along with them.
Tribal people have behavioural patterns of their own that tend to help the virus. They live close to each other in clusters and gather together for events. They have no understanding of mask-wearing and COVID-19 appropriate behaviour.
In fact, the problems here are not too dissimilar from those in urban areas except that the setting is vastly different and in the absence of communication there is no awareness. The tribal people are innocent.
Dr Rajkumar Ramasamy and his wife, Mary, run the KC Patty CF Primary Health Centre. It is a small voluntary effort which they have nurtured over two decades. Initially they would travel to KC Patty from Oddanchatram, where they were at the Christian Fellowship Hospital. Over time they based themselves in the village.
The Ramasamys are well-qualified. Rajkumar studied medicine at Cambridge and went on to become a Fellow of the Royal College of Physicians (FRCP). Mary is a gynaecologist trained at the Christian Medical College in Vellore.
Their health centre caters to a community of about 15,000 of whom around 6,000 come to the centre. The Ramasamys work on the principle that it is as important to reach patients where they are as it is to bring them to a facility.
They have at their centre a team of 12 who have been sourced from the local community and trained to be health workers and attendants. Being local, they connect with people and give them the confidence to seek treatment.
But it is not easy dealing with a deadly virus during a pandemic. When we spoke to the Ramasamys in end-April, they said that at least two deaths had occurred, one member of their team had been infected and another seemed to be infected.
Asked how many cases there were in the area, Dr Ramasamy says it is impossible to tell because there is no testing. In the absence of communication and a big enough primary care outreach, people don’t come forward to report a fever.
“There is this top-handed approach which I think scares people,” he says. “The local structures, like the panchayat and panchayat members, weren’t sufficiently involved.”
Though this is Tamil Nadu, with all its superior systems, in KC Patty there is no testing to speak of. To get a test done, a patient has to go to Dindigul or Oddanchatram, which inevitably means a bus ride and the possibility of infecting others.
There are also no facilities in the village for administering oxygen or treating cases that grow serious and need to be put in a hospital with life-saving capacities.
“We check the oxygen saturation. And if they’re okay, and it’s early symptoms only, then we treat them and manage them here. It is when the oxygen saturation falls that we have a problem,” explains Dr Mary Ramasamy.
“The patients who died had oxygen saturation that had dropped and so we had to call the government’s 108 number to come and take them to the government hospital,” she says.
Rajkumar adds: “It is standard protocol, what Mary is stressing on. The dilemma occurs because people don’t want to go anywhere. And then they are also often unable to go somewhere else.”
It is not as though getting to Dindigul, which is the nearest city, is a solution either. Patients with low saturation sent there are asked to wait in a queue and given oxygen for a few minutes every hour, the Ramasamys tell us.
 KC Patty’s angels: Dr Rajkumar Ramasamy (standing second from left) and Dr Mary Ramasamy (kneeling left) with members of their team at the KC Patty CF Health Centre
KC Patty’s angels: Dr Rajkumar Ramasamy (standing second from left) and Dr Mary Ramasamy (kneeling left) with members of their team at the KC Patty CF Health Centre
They say that the learning from the COVID-19 experience should be that primary healthcare services need to be strengthened. It is also important that secondary hospitals need to be better staffed and equipped with oxygen, beds and testing facilities. In this way primary health centres would have somewhere to readily send serious patients andthere would be no delay in attending to them.Lives would be saved.
Dr Rajkumar Ramasamy elaborates: “When the virus started, so much of the discussion was driven by the tertiary sector or highly specialized hospitals, or corporate health providers in cities. They were asking for ventilators and such things. There was very little stress on primary care when in reality that’s where the battle really needs to be fought and won.”
He believes things could have been different if doctors at the primary health centre level were professionally trained in family medicine and ASHAs were empowered and given the resources to serve meaningfully in their role as frontline workers.
“We should have the ASHAs and the panchayat members having discussions with the people in villages about this new virus, what are the symptoms, what we should worry about, and how you should use common sense to deal with it,” he says.
If that had been the approach, ASHAs would have been able to identify fevers and primary health centres would have had the facilities to conduct tests for COVID-19.
POLICY FAILURE
Well-qualified and talented doctors are needed to bolster primary healthcare and rural services in particular.
Rural outposts proffer good experience for young doctors. Dr Ashita Singh tells us that she first went to Chinchpada as an intern in 1998. The idea that young doctors and those who don’t make it in cities go to rural areas is a short-sighted one.
One reason for the lack of good doctors in rural areas is the failure of national policy. The government does little to improve conditions in its hospitals. It doesn’t provide the facilities that doctors need in rural areas. Living conditions are horrible and children can’t get a decent education.
The government also encourages a culture of super specialty medicine when what is needed and is in short supply is just dependable basic care.
Simultaneously, corporate hospitals flourish and lure talent in their direction. Medicine is increasingly studied to earn money and not to serve humanity. Medical education (and so many colleges are run by politicians) has been tailored to meet the commercial needs of this market.
When skilled doctors with advanced degrees go to rural areas there is inescapably the feeling of being excluded from the cutting edge of the profession — at least the way it is now structured.
Dr Iyengar talks of some in the profession being dismissive of the work done by a doctor like him as though it is peripheral and the result of not having succeeded in some mainstream capacity.
But where good doctors commit themselves to making a difference, they end up being inventive and impactful in ways that can hardly be imagined. They improve the lives of people. It is by choice that they serve far from the limelight and their satisfaction is in helping people who might not have otherwise got quality care.
Dr Mohan and Dr Iyengar have the qualifications to practise anywhere in the country. But they have shown through their efforts the difference midwifery and locally trained nurses can make to the health of women in the poor villages of southern Rajasthan.
Similarly, the Singhs at Chinchpada have made many things possible because of their training and skills. Dr Deepak Singh is a paediatric surgeon, with post-doctoral qualification, but he operates on a variety of cases. Some are simple general surgeries like a hernia and an appendix removal. Others have been more challenging such as reconstructing a bladder for a girl and giving her continence. He also does minimally invasive laparoscopic surgeries.
Dr Ashita Singh recalls the couple's early days in Chinchpada: “When we came to Chinchpada, the hospital was closed and we had to struggle to get the infrastructure going. There were days when Deepak would sit at the breakfast table and wonder what he was doing here as a paediatric surgeon.”
“You know, there are different ways of looking at cutting edge. There’s barely any paediatric surgery that actually comes here. But because of his paediatric surgery expertise, there are many simple things that get done to a very high standard,” she says. “And if you look at it, that actually results in life as against death, that results in people having a better outcome. What are we here for? We are here for people,” she explains.
Her degree in general medicine and training in palliative care has resulted in a palliative care programme for Chinchpada. It is tough to find palliative care in big cities, but Chinchpada has it thanks to the Singhs practising there.
Some 400 people have received palliative care at home in Chinchpada since 2016. The programme has also helped with the treatment of TB, which is a big local problem. A TB patient requires hand-holding. Palliative care arrangements will also be needed for cases of long COVID-19.
“The hospital gets a lot of TB patients. I think part of it is because TB needs a long-term relationship and a lot of care especially for people who are illiterate or don’t understand things. We also have a good partnership with the government for treatment of TB,” she says.
At Nadiad, a small city in Gujarat, Dr Sanjeeth Peter runs the DDMM Heart Institute. Around 300 surgeries a year are performed here. The success rate is 98 percent.
Dr Peter has been here for 20 years. The hospital has a big reputation locally. So, when COVID-19 came along people turned to it for treatment.
Faced with the problem of sourcing oxygen, Dr Peter came up with a redesign for an oxygen mask which reduced by as much as 50 percent the oxygen used by a patient in hospital conditions. The redesigned mask is now finding users all over the country.
“Cardiac surgeons are basically plumbers. Fixing pipes and channels is what we know to do,” says Dr Peter, who took only 10 minutes to figure out what was wrong with the design of the original Non Re-breathable Mask (NRBM) when used under the stressful circumstances of the pandemic.
Even as innumerable patients died for want of oxygen in big cities during the second wave, many rural hospitals had already found their own solutions.
It was partly due to the focus and dedication of doctors running such establishments and also because of having to live up to challenges over the years.
At the Makunda Hospital in Assam, close to the border with Tripura, there was a time when oxygen cylinders used to arrive by boat. The closest city is Karimganj.
But the hospital dealt with the problem squarely and over the years installed two oxygen plants, which is something many hospitals in big cities didn’t have as they struggled to cope with cases in the second wave.
BACK TO BASICS
Improving healthcare facilities in India will require a return to basics. Experience shows that there is no substitute for a better primary healthcare system. It is important to restore the values of the medical profession and make it more relevant to the realities of a largely poor and uneducated country.
It is necessary to engage more with the voluntary sector so as to learn from its vast and valuable experience and also allow public-spirited doctors to play a bigger role as leaders. A new generation of doctors, nurses and medical attendants should be put in place.
Governments at the centre and in the states have the responsibility for introducing a new order of priorities. The pandemic has shown that years of neglect have proved to be costly.
Comments
-

Dr G Buvaneswari - July 5, 2021, 10:51 p.m.
Excellent services. It needs lots of courage and dedication to stay in rural areas after studying and working in tertiary centres. All the best .
-

Dr.anita Varghese - July 5, 2021, 5:20 p.m.
Your story was really an insight into how the selfless dedication and passion of highly qualified doctors is making a difference to the lives of rural and tribal people. It is by no means an easy task to win their trust and faith. It is all the more difficult in these difficult and pandemic times to carry on such work with limited resources and to update or upscale using limited resources to meet the situation headlong. My salute to these real heroes. God bless.
-

Jaydeb Rana - June 27, 2021, 11:03 p.m.
Excellent
-

Dr Santanu Tripathi - June 25, 2021, 10:02 a.m.
Great article. Great initiatives. Deserves a reading by all concerned with health care delivery. Particularly the policy makers. Time to think afresh. Time to make care delivery inclusive ensuring access by all. Let this article be reproduced in mainstream media.
-

Dr V Chandra-Mouli - June 23, 2021, 10:59 a.m.
Congrats for a great article featuring the inspirational work of both religious and secular organizations striving to provide high quality clinical care with empathy and sensitivity, making the best use of available resources.
-

Robin Thomson - June 21, 2021, 6:40 p.m.
A great article. It shows the importance of primary health care and the difference it makes when (a) skilled doctors commit themselves to reach out into the community and (b) they empower and mobilise local people to provide care right at the local level, backed up by the doctors' support from behind. This model is transformational and I have seen other examples during my time in India (not as a medical/health person). Why doesn't it happen more often? It takes commitment, trust and willingness of the skilled people to use their skills to empower others.
-

evita fernandez - June 21, 2021, 1:11 p.m.
Thank you, for this article that featured the real heroes of our country. The healthcare teams working in rural India, serving the underprivileged in a holistic manner. My gratitude to these doctors who have set up NGOs and who are working in rural hospitals- may their tribe increase.
-

Kimi Archer - June 19, 2021, 7:36 p.m.
Excellent article! Thank you!
-

Dr.Nepuni Athikho - June 19, 2021, 7:18 a.m.
It very heart warming to see my mentor and his team in the villages. Both Dr. Deepak and Ashita are the backbone of mission hospitals. Their dedicated service shows how much they love and care for the poor and needy. I praise God for them.



